Home / Training / Manuals / Atlas of breast cancer early detection / Cases
Atlas of breast cancer early detection
Filter by language: English / Русский
Go back to the list of case studies
.png) Click on the pictures to magnify and display the legends
Click on the pictures to magnify and display the legends
| Case number: | 095 |
| Age: | 58 |
| Clinical presentation: | Postmenopausal woman with average risk of developing breast cancer presented with a lump in the left breast. Examination revealed a 1.5 cm lump in the retroareolar region of the left breast. |
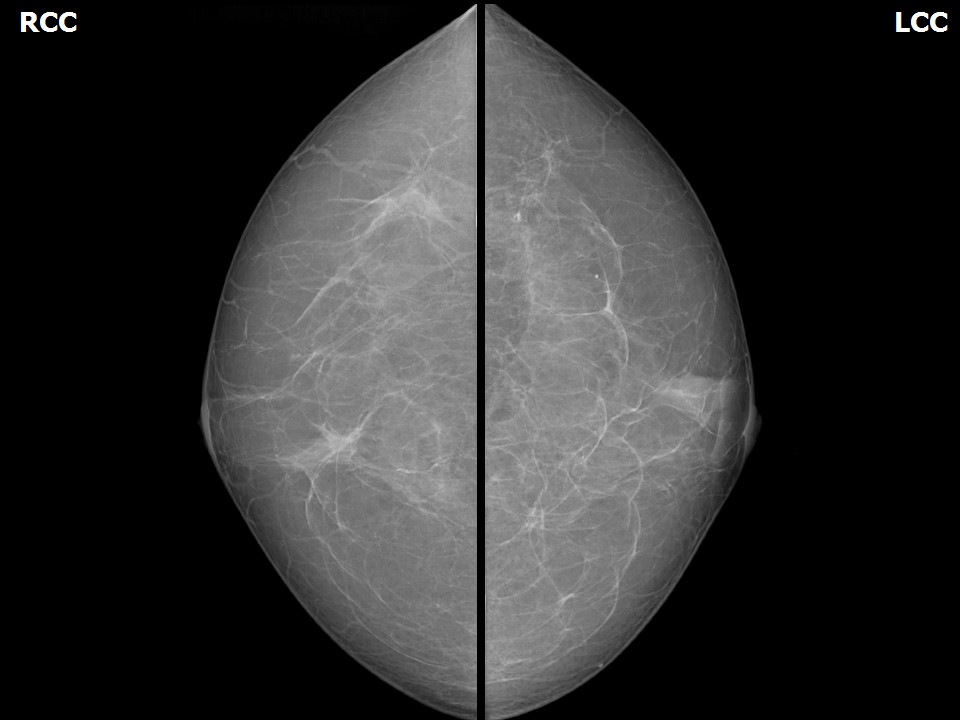
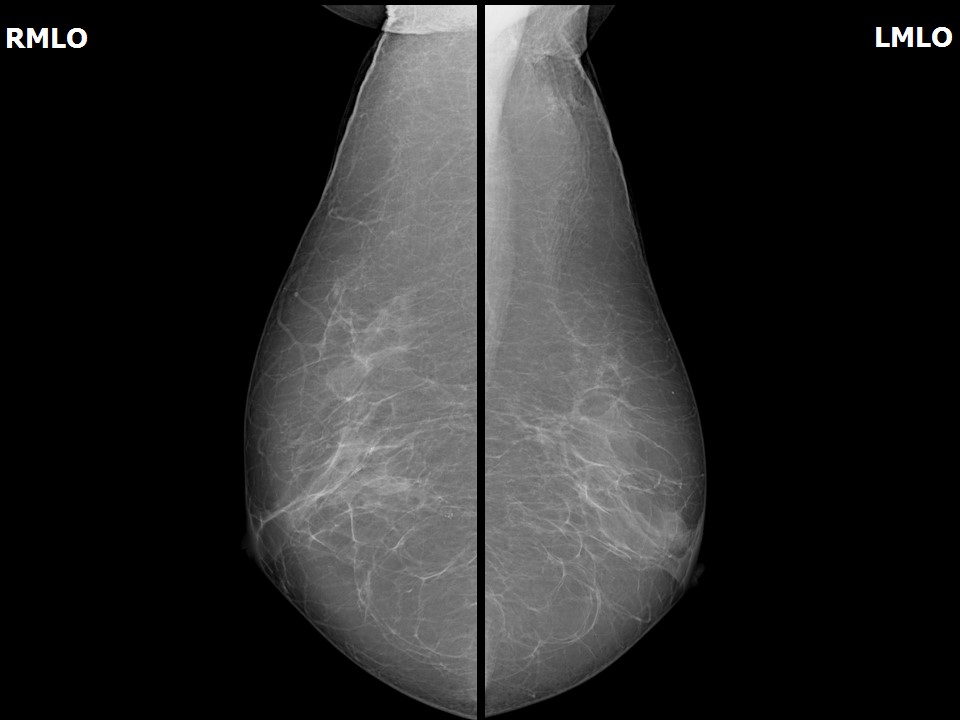
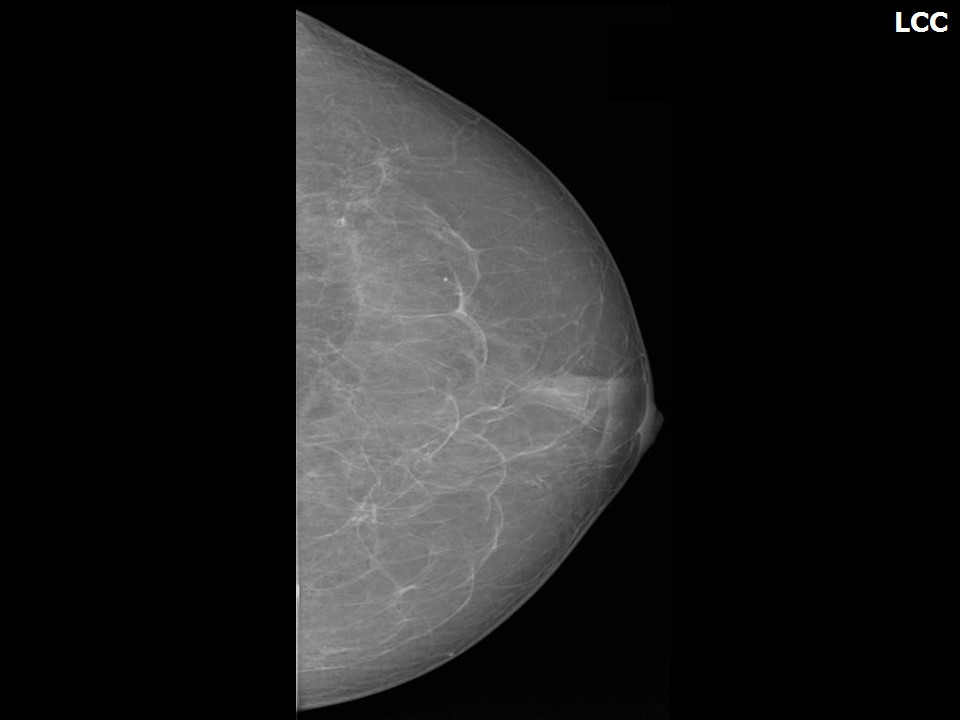
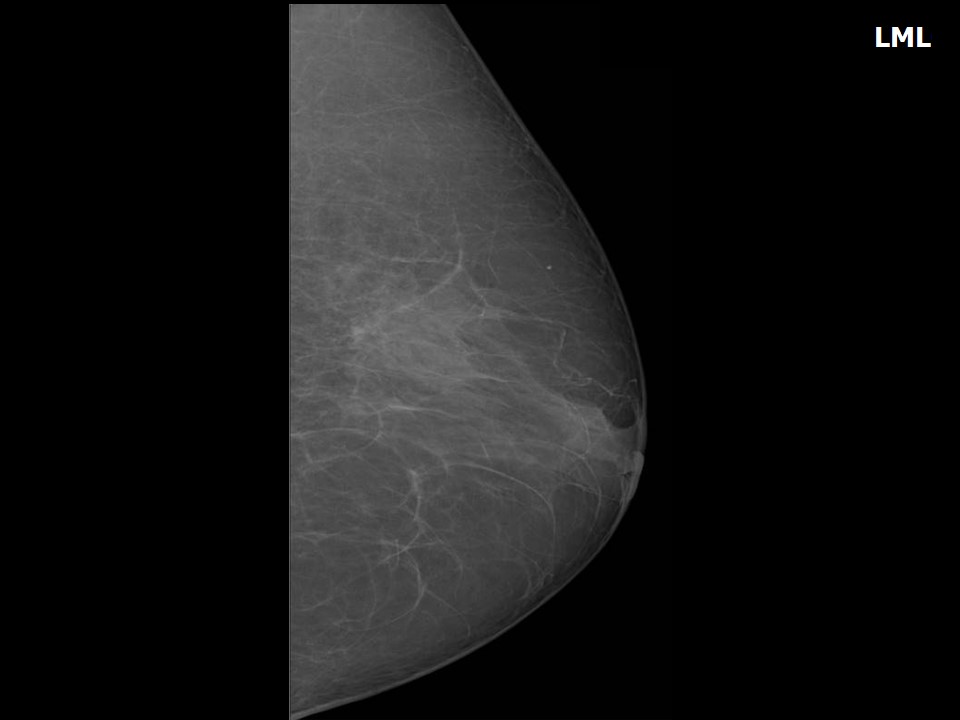
Mammography:
| Breast composition: | ACR category a (the breasts are almost entirely fatty) | Mammography features: |
| ‣ Location of the lesion: | Left breast, central portion of the breast, central zone, anterior third |
| ‣ Mass: | |
| • Number: | 1 |
| • Size: | 1.2 × 0.9 cm |
| • Shape: | Irregular |
| • Margins: | Indistinct |
| • Density: | Equal |
| ‣ Calcifications: | |
| • Typically benign: | None |
| • Suspicious: | None |
| • Distribution: | None |
| ‣ Architectural distortion: | None |
| ‣ Asymmetry: | None |
| ‣ Intramammary node: | None |
| ‣ Skin lesion: | None |
| ‣ Solitary dilated duct: | None |
| ‣ Associated features: | None |
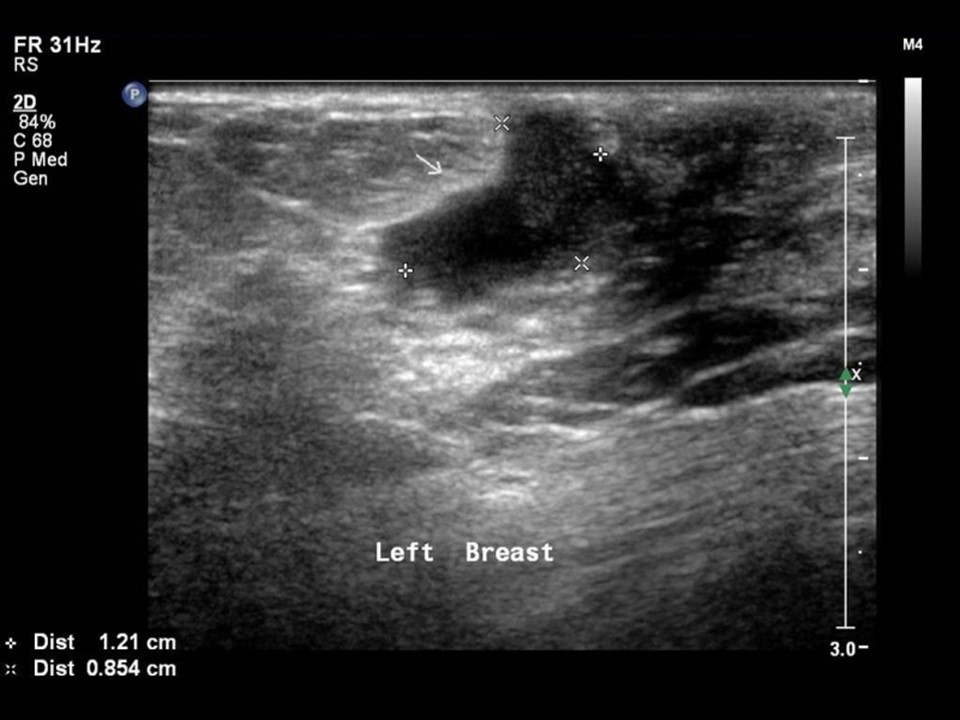
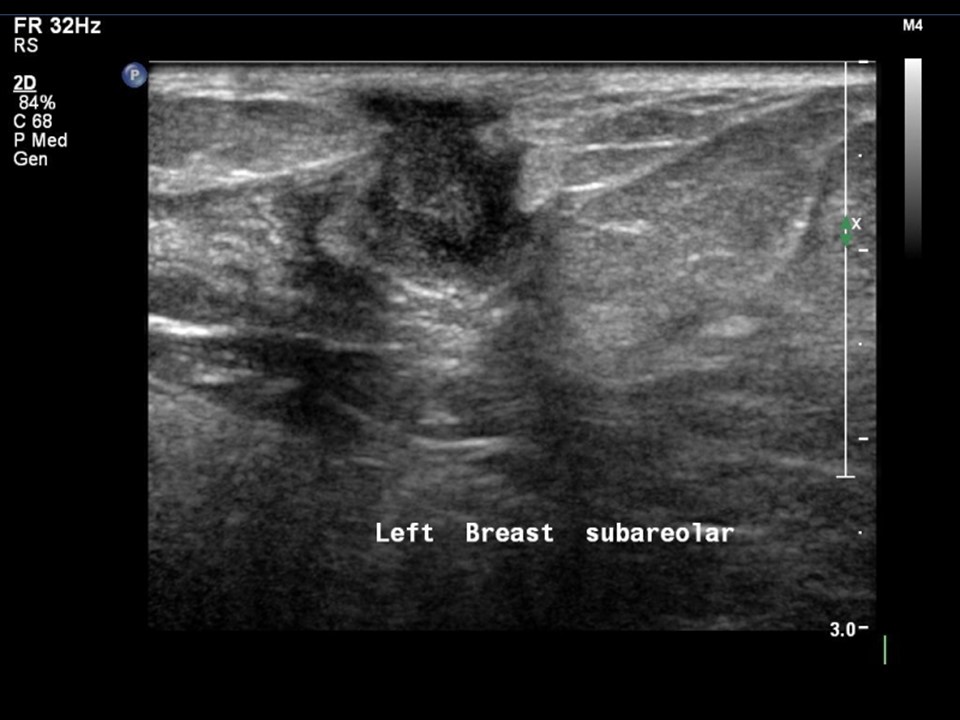
Ultrasound:
| Ultrasound features: Left breast, central portion of the breast | |
| ‣ Mass | |
| • Location: | Left breast, central portion of the breast |
| • Number: | 1 |
| • Size: | 1.2 × 0.8 cm |
| • Shape: | Irregular |
| • Orientation: | Not parallel |
| • Margins: | Indistinct |
| • Echo pattern: | Heteroechoic |
| • Posterior features: | No posterior features |
| ‣ Calcifications: | None |
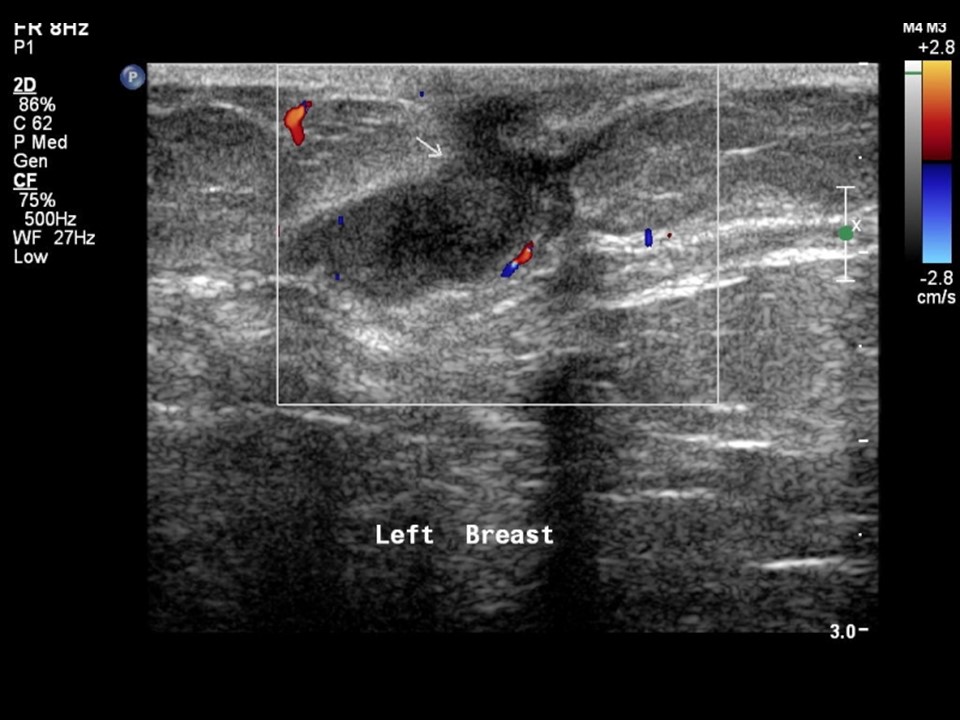
| ‣ Associated features: | Vessels in rim |
| ‣ Special cases: | None |
BI-RADS:
BI-RADS Category: 4A (low level of suspicion for malignancy)Further assessment:
Further assessment advised: Referral for cytologyCytology:
| Cytology features: | |
| ‣ Type of sample: | FNAC (solid lesion) |
| ‣ Site of biopsy: | |
| • Laterality: | Left |
| • Quadrant: | Retroareolar lump |
| • Localization technique: | Palpation |
| • Nature of aspirate: | 0.2 mL of thick whitish material |
| ‣ Cytological description: | Smear shows many neutrophils and foamy macrophages. Epithelioid histiocytes are seen in large conglomerates |
| ‣ Reporting category: | Benign |
| ‣ Diagnosis: | Granulomatous inflammation |
| ‣ Comments: | None |
Histopathology:
Breast lumpectomy
| Histopathology features: | |
| ‣ Specimen type: | Breast lumpectomy |
| ‣ Laterality: | Left |
| ‣ Macroscopy: | Cut surfaces of the serial sections do not show any tumour nodules. Soft whitish areas are noted in the adipose tissue |
| ‣ Histological type: | Section shows granulomatous mastitis with epithelioid cell conglomerates, Langhans giant cells, and peripheral cuff of lymphocytes. Some dilated ducts with inspissated secretions and surrounded by chronic inflammation are seen |
| ‣ Histological grade: | |
| ‣ Mitosis: | |
| ‣ Maximum invasive tumour size: | |
| ‣ Lymph node status: | |
| ‣ Peritumoural lymphovascular invasion: | |
| ‣ DCIS/EIC: | |
| ‣ Margins: | |
| ‣ Pathological stage: | |
| ‣ Biomarkers: | |
| ‣ Comments: | Negative for acid-fast bacilli |
Case summary:
| Postmenopausal woman presented with left breast lump. Diagnosed as left breast subareolar tubular irregular lesion, BI-RADS 4A on imaging and as granulomatous mastitis on cytology and histopathology. |
Learning points:
|