Introduction
Different approaches to screening and treatment of cervical precancer
Anatomical considerations
Physiological changes of the cervical epithelium
Neoplastic changes of the cervical epithelium
HPV tests Variation between tests
Instruments, consumables, and setup required
Procedure to collect samples for HPV testing
Interpretation of HPV test results
Management of women with a positive HPV test result
Treatment of cervical intraepithelial neoplasia principles
Steps to determine eligibility for ablative treatment
Role of Lugols iodine in identifying the transformation zone for treatment
Treatment by cryotherapy
Treatment by thermal ablation
Using an HPV test as the test of cure in women treated for cervical abnormalities or cervical intraepithelial neoplasia (CIN)
Infection prevention
Case studies
VIA triage outcome (applicable in screen-and-treat setting only) negative cases
VIA triage outcome positive cases
VIA triage outcome suspicious of cancer cases
Foreword
Acknowledgement
Authors
Suggested citation
Copyright
Home / Training / Manuals / Using HPV tests for cervical cancer screening and managing HPV-positive women a practical online guide / Learning
Using HPV tests for cervical cancer screening and managing HPV-positive women a practical online guide
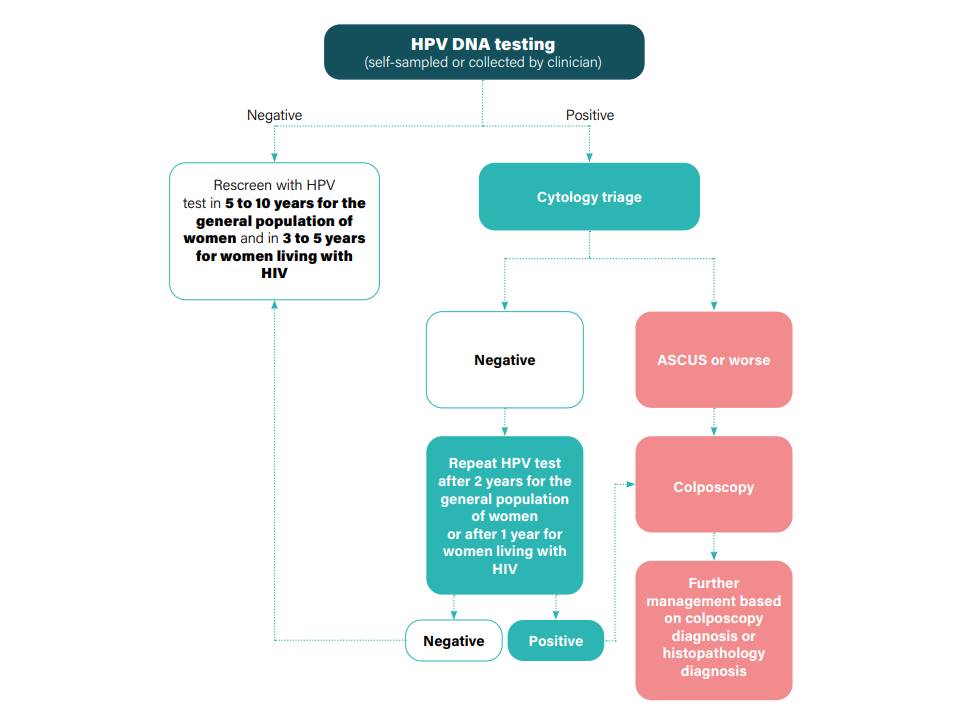
Filter by language: English / Français / EspañolManagement of women with a positive HPV test result Triage with cytology | Click on the pictures to magnify and display the legends |
This section describes the algorithm for managing an HPV-positive woman with Pap smear cytology. If the sample was collected by a health provider from the cervix in an appropriate transport medium (e.g. in a tube containing PreservCyt, SurePath, or Roche medium), then the same sample may be used for liquid-based cytology. The woman need not be recalled. However, liquid-based cytology is not feasible on self-collected specimens or on specimens that were not collected in an appropriate medium. In such cases, the woman needs to be recalled for the collection of another sample by a provider. The same applies in settings with facilities for conventional Pap smear but not liquid-based cytology. Women with abnormal cytology are referred for colposcopy. The colposcope enables examination of the cervix under a good light source and with different levels of magnification. Depending on the results of the colposcopic examination, a colposcopist may decide to either take a biopsy from the abnormal area or proceed directly to treatment. HPV-positive women with a normal colposcopy result should be reassured and advised to have a repeat HPV test after 2 years. The HPV test is to be repeated after 1 year in women living with HIV.
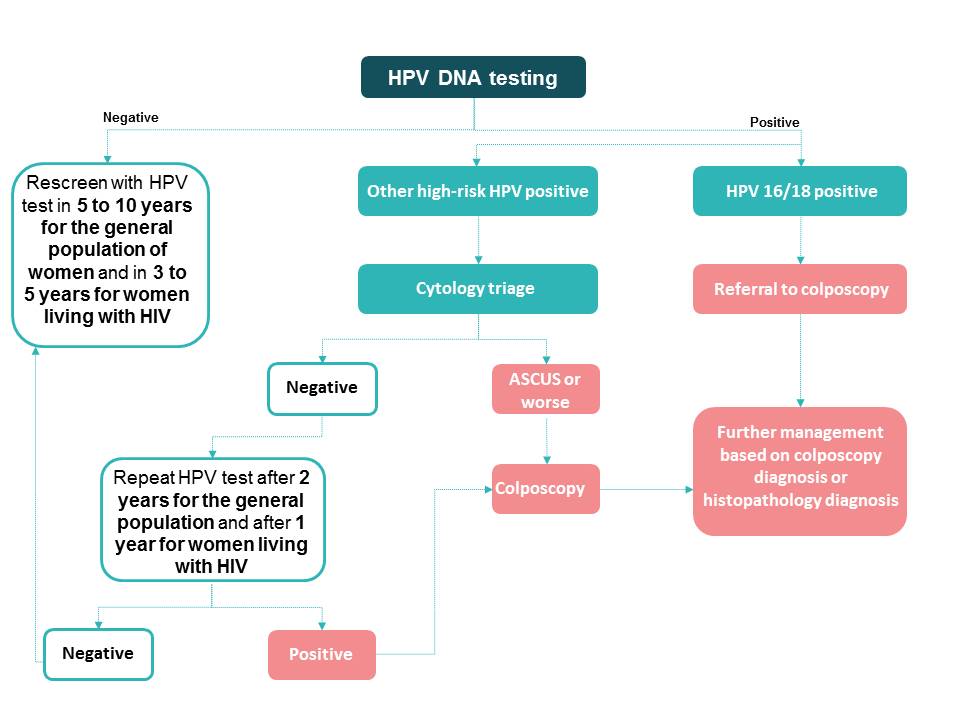
To learn more about colposcopy, access the Atlas of Colposcopy: Principles and Practice. The algorithm may be slightly different when partial genotyping information is provided simultaneously by the HPV test. Women who are known to be positive for HPV16 or HPV18 may be directly referred for colposcopy, whereas those who test positive for other high-risk HPV types undergo cytology for triage. In either algorithm, women with no abnormalities detected on cytology are advised to have a repeat HPV test after 2 years, and those who test positive on the repeat HPV test are directly referred for colposcopy. The HPV test is to be repeated after 1 year in women living with HIV. |
IARC, 150 Cours Albert Thomas, 69372 Lyon CEDEX 08, France - Tel: +33 (0)4 72 73 84 85 - Fax: +33 (0)4 72 73 85 75
© IARC 2025 - All Rights Reserved.
© IARC 2025 - All Rights Reserved.