Image | Caption |
 | Figure 1A: Physical examination under bright daylight. |
 | Figure 1B: Oral examination using head mirror. |
 | Figure 1C: Oral examination with torch and wooden spatula. |
 | Figures 2: Examination of the lips. |
 | Figure 3: Examination of the labial mucosa. |
 | Figures 4: Examination of the buccal mucosa. Buccal mucosa is examined by retracting it with wooden spatulas or mouth mirrors, after the subject opens the mouth partially in a relaxed position. |
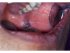 | Figure 5: Linea alba buccalis. Note the linear, white, keratotic fold (arrow) on the left buccal mucosa that runs parallel to the occlusal plane. |
 | Figure 6: Fordyce granules (arrows). Note the small yellowish nodules on the right buccal mucosa. |
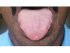 | Figure 7: The dorsal surface of the tongue is examined by asking the person to protrude the tongue and attempt to touch the tip of the chin. |
 | Figure 8: The tip of the tongue may be held gently by the fingers and a gauze sponge. |
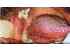 | Figure 9: The lateral borders of the tongue are examined by grasping the tip of the tongue with a gauze sponge, extending and rotating it laterally. |
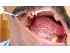 | Figure 10: The lateral border of the tongue can be examined by asking the person to touch the opposite buccal mucosa with the tip of the tongue and retracting the buccal mucosa with a mouth mirror. |
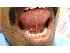 | Figure 11: The ventral surface of the tongue and the floor of the mouth are most easily visualized by having the person touch the roof of the mouth with tip of the tongue. |
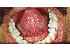 | Figure 12: Opening of Wharton duct (yellow arrows). |
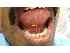 | Figure 13: Median frenum of tongue (yellow arrow). |
 | Figure 14A: The gingivae are examined with the mouth partially opened and lips retracted with mouth mirrors. |
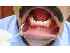 | Figure 14B: Examination of the gingivae is carried out with the mouth partially opened and the lips retracted with mouth mirrors. |
 | Figure 15: The anterior part of the hard palate is better visualised using a mouth mirror. |
 | Figure 16: The soft palate is examined by depressing the base of the tongue with a mouth mirror and asking the subject to say aah. |
 | Figure 17: The examination for cervical lymph nodes is carried out by standing behind the individual and slightly flexing and bending the neck to the side so that the sternocleidomastoid muscle becomes relaxed and palpation and identification of any enlarged nodes will be easier. |
 | Figure 18A: Patient with enlarged metastatic right upper deep cervical lymph node on the right side (arrow). |
 | Figures 18A and 18B: Pleomorphic adenoma of the right parotid gland. The ear lobule is pushed upwards and backwards by the tumour, which helps to differentiate parotide tumour from enlarged upper deep cervical lymph node. |
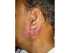 | Figure 19: Carcinoma of the left parotide gland infiltrating the overlying skin. |