Image | Caption |
 | Table 1: Points to consider prior to mucosal biopsy adapted from Oliver et al., 2004. 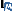 . . |
 | Table 2: Guidelines for an appropriate biopsy adapted from Oliver et al., 2004. 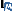 . . |
 | Figure 1: Instruments needed for biopsy procedure: A: reusable punch biopsy forceps, B: disposable punch forceps, C: needle holding forceps, D: thumb forceps, E: scissors, F: artery forceps, G: Bard-Parker knife. |
 | Figures 2A and 2B: Incision biopsy procedure. Biopsy being taken from the edge of the lesion including a wedge of normal tissue. |