Image | Caption |
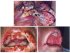 | Figure 1A: Advanced exophytic proliferative growth involving the whole left buccal mucosa, left side of both upper and lower lips and adjacent skin. Figure 1B: Picture of the same patient taken at the end of chemoradiotherapy showing confluent mucosal ulcerations of the oral cavity. C: Picture of the same patient taken 2 months after chemoradiotherapy. |
 | Figure 2: Osteoradionecrosis of left side of the mandible. Note the necrotic exposed area of the left mandible one year following radiotherapy for carcinoma of the left alveolus. |
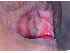 | Figure 3: Radiation mucositis of the left buccal mucosa 10 days after interstitial implantation. |
 | Figure 4: Acute radiation mucositis at the end of the radiotherapy treatment in a patient with carcinoma of the left buccal mucosa. |
 | Figure 5: Note the discharging sinus (arrow) on the left side of the lower jaw due to osteoradionecrosis in a patient who underwent surgery and radiotherapy four years earlier. There is no evidence of malignancy now. |
 | Figure 6: Osteoradionecrosis of right side of the mandible in a patient six years after radiotherapy. |
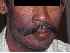 | Figure 7: Dry desquamation of the skin (acute reaction) on the right side of the face of a patient undergoing external radiotherapy for carcinoma of right buccal mucosa. |
 | Figure 8: Dry desquamation (acute reaction) of the neck in a patient who recently completed radiotherapy treatment. |
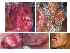 | Figures 9A and 9B: Ulceroproliferative growth involving the whole of the left buccal mucosa infiltrating the overlying skin. Figures 9C and 9D: Treatment response one month after radiotherapy. Figure E: Treatment response 3 years after radiotherapy. |
 | Figure 10: Acute radiation mucositis. Confluent yellowish mucosal ulcer seen on the left side of buccal muccosa in a patient who completed external beam radiotherapy for a carcinoma of the left buccal mucosa. |