Image | Caption |
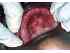 | Figure 1: Chronic atrophic candidiasis (denture sore mouth). Note the diffuse erythema involving the entire hard palate due to the use of the same dentures for the past 20 years. |
 | Figure 2: Chronic atrophic candidiasis. Note the atrophic area in the hard palate and in the upper labial sulcus due to prolonged use of the same dentures for the past 16 years. |
 | Figure 3: Chronic atrophic candidiasis. A: Note the central papillary atrophy in the dorsum of tongue. B: Note the erosive area in the palate. |
 | Figure 4: Denture sore mouth: Edentulous patient who has dentures worn for 8 years having erythematous areas in the hard palate commonly attributed to candidal infection. |
 | Figure 5: Central papillary atrophy of the tongue (chronic atrophic candidiasis). Note the papillary atrophy in the mid part of dorsum tongue with multiple lobular and fissured appearance. |
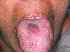 | Figure 6: Central atrophic candidiadis. Note the 2x2 cm atrophic area in the mid part of the dorsum of tongue in this 38year-old woman. |
 | Figure 7: Acute pseudomembranous candidiasis: Note the curdy-white flecks on an erythematous base. The white flecks can be removed by gentle rubbing or scrapping the mucosa which reveals an area of erythema. |
 | Figure 8: Acute pseudomembranous candidiasis on the left buccal mucosa. |
 | Figure 9: Acute candidiasis in a patient with oral submucous fibrosis. |
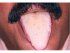 | Figure 10: Coated tongue. Note the diffuse coating on the dorsum of the tongue. Scraping from dorsum tongue showed candidial hyphae. |
 | Figure 11: Acute pseudomembranous candidiasis. |