Home / Training / Manuals / Colposcopy and treatment of cervical intraepithelial neoplasia: a beginners manual / Chapter 5: The Colposcopic Examination Step-by-Step
 figure 4.6: Endocervical speculum<...
figure 4.6: Endocervical speculum<...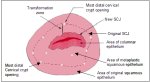 FIGURE 5.1: A method of identifyin...
FIGURE 5.1: A method of identifyin...
 figure 4.8: Cervical punch biopsy ...
figure 4.8: Cervical punch biopsy ...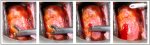 figure 5.2: Biopsy technique: A to...
figure 5.2: Biopsy technique: A to...
 figure 4.7: Endocervical curette
figure 4.7: Endocervical curette
Colposcopy and treatment of cervical intraepithelial neoplasia: a beginners manual, Edited by J.W. Sellors and R. Sankaranarayanan
Chapter 5: The Colposcopic Examination Step-by-Step
Filter by language: English / Français / Español / Portugues / 中文- It is important to explain the examination procedure and reassure the woman before colposcopy. This will ensure that the woman relaxes during the procedure.
- Written informed consent should be obtained from the woman before the colposcopic examination.
- Relevant medical and reproductive history should be obtained before the procedure.
- A strict adherence to the essential steps involved in colposcopic examination ensures that common errors are avoided.
- It is important to visualize the squamocolumnar junction in its entire circumference, otherwise, the colposcopic procedure is termed unsatisfactory.
- One should identify the transformation zone (TZ) during the colposcopic procedure. The proximal limit of the TZ is defined by the squamocolumnar junction, while the distal limit of the transformation zone is identified by finding the most distal crypt openings or nabothian follicles in the lips of the cervix and by drawing an imaginary line connecting these landmarks.
- It is essential to obtain directed biopsies, under colposcopic control, from abnormal/-suspicious areas identified. Colposcopy during pregnancy requires considerable experience. As pregnancy progresses, cervical biopsy is associated with increased probability and severity of bleeding, which is often difficult to control. The risk of biopsy should always be weighed against the risk of missing an early invasive cancer. Non-invasive lesions may be evaluated post-partum.
The steps involved in colposcopic examination to identify cervical neoplasia are described in detail in this chapter. A strict adherence to this examination protocol ensures that common errors in colposcopic practice are avoided to a large extent. It is advised that students should have thoroughly reviewed the anatomical and pathophysiological basis of colposcopic practice described in the previous chapters before going any further.
Practise first on inanimate objects
The colposcope can be thought of as an extension of the clinicians visual sense; as such, with practice, it should become a familiar tool rather than an impediment - a part of the colposcopists body, so to speak. When one is learning colposcopy, it is helpful to become familiar with the equipment that one will be using. It is a good idea to practise focusing on inanimate objects (such as apples, oranges, flowers, small bottles with labels, etc.) in the examining room, using different light intensities and magnifications, with and without the green and/or blue filter.
Two adjustments may be required to personalize the instrument for use. The instrument should be adjusted to suit the interpupillary distance of the colposcopist to achieve stereoscopic vision by altering the separation between the two ocular lenses (eyepieces). The eyepieces should be kept wide open initially. If when looking through the colposcope, one can see two separate fields of vision, the eyepieces should be brought closer until the two fields merge to give a stereoscopic binocular vision. The eyepieces can also be adjusted to compensate for variation in an individual colposcopists vision by changing the focus of each ocular lens, which can be matched to the correction required (+ or - dioptres), if any, by using the dioptre scale on the side of the eyepieces. This is achieved by looking through the right eyepiece with the left eye closed and moving the colposcope and by tuning the fine focus using the fine focus handle so that the image comes into focus. Without moving the colposcope, and closing the right eye, the left eyepiece should then be turned slowly until the image comes into focus. Now the instrument has been adjusted to suit the individuals vision. Those with normal eyesight or eyesight corrected by glass need not do any correction of dioptre setting.
One method of practising colposcopic biopsy technique on an inanimate object involves using a piece of pipe that matches the diameter and length of the vagina (about 5 cm wide and 15 cm long) and a foam rubber ball that can be cut into sections and wedged into the distal end of the pipe. Typewriter correction fluid or similar paint can be used to simulate lesions on the surface of the foam rubber. These painted lesions form the targets with which to practise colposcopy. This avoids the problem of procuring animal tissues on which to practise and the attendant problems of storing and cleaning them up. Biopsies should be done under colposcopic visualization whenever possible, so the biopsy technique should be learned using the colposcope. Whenever possible the student should be under the supervision of an instructor who is experienced in colposcopy and, if possible, has taken a training course. Interactive learning, based on actual patients, will accelerate the learning curve. In practice sessions, it is worthwhile learning to use colposcopy assessment forms (see Appendix 1) to document the findings and the location where a biopsy has been taken.
Two adjustments may be required to personalize the instrument for use. The instrument should be adjusted to suit the interpupillary distance of the colposcopist to achieve stereoscopic vision by altering the separation between the two ocular lenses (eyepieces). The eyepieces should be kept wide open initially. If when looking through the colposcope, one can see two separate fields of vision, the eyepieces should be brought closer until the two fields merge to give a stereoscopic binocular vision. The eyepieces can also be adjusted to compensate for variation in an individual colposcopists vision by changing the focus of each ocular lens, which can be matched to the correction required (+ or - dioptres), if any, by using the dioptre scale on the side of the eyepieces. This is achieved by looking through the right eyepiece with the left eye closed and moving the colposcope and by tuning the fine focus using the fine focus handle so that the image comes into focus. Without moving the colposcope, and closing the right eye, the left eyepiece should then be turned slowly until the image comes into focus. Now the instrument has been adjusted to suit the individuals vision. Those with normal eyesight or eyesight corrected by glass need not do any correction of dioptre setting.
One method of practising colposcopic biopsy technique on an inanimate object involves using a piece of pipe that matches the diameter and length of the vagina (about 5 cm wide and 15 cm long) and a foam rubber ball that can be cut into sections and wedged into the distal end of the pipe. Typewriter correction fluid or similar paint can be used to simulate lesions on the surface of the foam rubber. These painted lesions form the targets with which to practise colposcopy. This avoids the problem of procuring animal tissues on which to practise and the attendant problems of storing and cleaning them up. Biopsies should be done under colposcopic visualization whenever possible, so the biopsy technique should be learned using the colposcope. Whenever possible the student should be under the supervision of an instructor who is experienced in colposcopy and, if possible, has taken a training course. Interactive learning, based on actual patients, will accelerate the learning curve. In practice sessions, it is worthwhile learning to use colposcopy assessment forms (see Appendix 1) to document the findings and the location where a biopsy has been taken.
Steps in the colposcopic examination
Many authors have provided good advice about the proper way to conduct a colposcopic examination ( Campion et al., 1991; Cartier & Cartier, 1993; Coppleson et al., 19.3; Soutter 1993; Wright et al., 19.5; Anderson et al., 1996; Burghart et al., 1998; Singer & Monaghan 2000). Though there are different schools of thought and practice of colposcopy, the approach discussed in this manual is based on the classical or extended colposcopy technique.
Colposcopists often form their own judgements regarding what they believe is essential to the colposcopic examination, and discard much of what they deem not to be useful. It seems that colposcopic practice is somewhat flexible in content and the order of performance of different steps may vary in different settings, since circumstances change according to cultural and other contextual settings in which colposcopy is conducted worldwide. However, we recommend that the following steps be carefully followed during the learning phase, as well as during routine colposcopic practice. Wherever possible, we have given the reason for each step. Often the evidence for the value of each step will come with experience. The evaluation of normal and abnormal colposcopic findings is given in Chapters 6 to 9.
Colposcopists often form their own judgements regarding what they believe is essential to the colposcopic examination, and discard much of what they deem not to be useful. It seems that colposcopic practice is somewhat flexible in content and the order of performance of different steps may vary in different settings, since circumstances change according to cultural and other contextual settings in which colposcopy is conducted worldwide. However, we recommend that the following steps be carefully followed during the learning phase, as well as during routine colposcopic practice. Wherever possible, we have given the reason for each step. Often the evidence for the value of each step will come with experience. The evaluation of normal and abnormal colposcopic findings is given in Chapters 6 to 9.
Explain the procedure to the woman
Women referred to a colposcopy clinic may not have had the procedure explained to them in detail before their arrival. For literate women, pamphlets on what an abnormal cervical cytology or other screening test means and an explanation of the colposcopic examination may be helpful. It is important for all women to have a prior explanation of the procedure and reassurance by the clinic nurse or the colposcopist. Colposcopic examination may prove difficult and yield suboptimal results if the woman does not relax during the procedure. Privacy during the consultation and examination is of utmost importance.
Obtain informed consent
After the procedure has been explained to the woman, written informed consent should be obtained, before colposcopy. The written consent form should include information about the colposcopic examination and the usual procedures that may accompany it, such as biopsy, endocervical curettage and photography, and summarize the usual complications (less serious and more frequent ones, as well as more serious but less frequent ones) that may occur. An example of a written informed consent form is given in Appendix 2. It may be preferable to obtain informed consent each time, if a woman requires subsequent colposcopic examinations.
Treatment for a colposcopically confirmed cervical intraepithelial neoplasia (CIN) may be planned during the same visit as colposcopy, to minimize the number of visits and to ensure compliance with treatment, as women may not be willing (for a variety of reasons) to make a subsequent visit to complete treatment. An ablative treatment like cryotherapy (see Chapter 12) may be planned after directing a biopsy during colposcopy (so that histopathology results for the treated lesion will be available at a later date). On the other hand, an excisional treatment such as loop electrosurgical excision procedure (LEEP) (see Chapter 13) will produce a tissue specimen that will help to establish the pathological nature of the lesion treated. If such an appproach to treatment immediately after colposcopy in the same visit is planned, the informed consent process should deal with treatment issues as well. The possible consequences of this approach in terms of overtreatment or unnecessary treatment, as well as the potential side-effects and complications of the treatment procedure, should be explained before obtaining the informed consent.
Treatment for a colposcopically confirmed cervical intraepithelial neoplasia (CIN) may be planned during the same visit as colposcopy, to minimize the number of visits and to ensure compliance with treatment, as women may not be willing (for a variety of reasons) to make a subsequent visit to complete treatment. An ablative treatment like cryotherapy (see Chapter 12) may be planned after directing a biopsy during colposcopy (so that histopathology results for the treated lesion will be available at a later date). On the other hand, an excisional treatment such as loop electrosurgical excision procedure (LEEP) (see Chapter 13) will produce a tissue specimen that will help to establish the pathological nature of the lesion treated. If such an appproach to treatment immediately after colposcopy in the same visit is planned, the informed consent process should deal with treatment issues as well. The possible consequences of this approach in terms of overtreatment or unnecessary treatment, as well as the potential side-effects and complications of the treatment procedure, should be explained before obtaining the informed consent.
Obtain a relevant medical history
The womans medical history is usually taken after her written informed consent has been obtained. Most women are referred after a screening examination and it is ideal to have the result of the screening test available at the time of colposcopic examination. If the woman has been referred because of abnormal cytology results, it is ideal to have a written copy of the previous smear(s) on hand at the time of the colposcopy appointment. Relevant obstetric and gynaecological history and history of any relevant exposures (e.g., number of pregnancies, last menstrual period, history of oral contraceptive use, hormonal supplements, sexually transmitted infections, etc.) should be obtained and recorded with the aid of a form designed for this purpose. It is important to enquire about the last menstrual period in order to assess the possibility of pregnancy or menopause.
Insert the vaginal speculum and inspect the cervix
The woman should be in a modified lithotomy position on an examining table with heel rests, or stirrups or knee crutches. It is preferable to place the buttocks slightly over the end of the table. It is important to ask the woman to relax. Positioning the buttocks in this way makes it much easier to insert the speculum and to manipulate it in different axes, if needs be. An instrument tray with essential instruments for colposcopy is placed beside the couch (Figure 4.3). A medium-size bivalve speculum (Cusco, Grave, Collins or Pedersens) is usually adequate. Warm, clean water on the speculum is the preferred lubricant, as it warms the metal, but does not interfere with the interpretation of cervical specimens, such as a cytology smear. If the woman has extremely lax vaginal walls, a lateral vaginal side-wall retractor (Figure 4.5) or a latex condom on the speculum (with the tip of the condom cut 1 cm from the nipple) is helpful (Figure 4.9). Particular care should be taken to align the blades of the vaginal side-wall retractor perpendicular to the vaginal speculum to prevent vaginal pinching. The skills for this manoeuvre come with practice. In very obese women, it may be preferable to use two Sims specula to retract the anterior and posterior vaginal walls.
Once the speculum is inserted and the blades are widely separated, a good view of the cervix and the vaginal fornices is obtained. This may also result in some eversion of the lips of the multiparous cervix, allowing the lower portion of the endocervical canal to come into view. After exposing the cervix, one should assess the nature of the cervico-vaginal secretions and note any obvious findings such as ectropion, polyp, nabothian follicles, congenital transformation zone, atrophy, inflammation and infection, leukoplakia (hyperkeratosis), condylomata, ulcer, growth and any obvious lesions in the vaginal fornices. Following this, excess mucus should be removed gently from the cervix with saline-soaked cotton swabs. Swabbing with dry cotton balls is discouraged, as these may induce traumatic bleeding and subepithelial petechiae. Loss of epithelium and bleeding due to rough and traumatic manipulation of the speculum and swabs should be avoided.
Once the speculum is inserted and the blades are widely separated, a good view of the cervix and the vaginal fornices is obtained. This may also result in some eversion of the lips of the multiparous cervix, allowing the lower portion of the endocervical canal to come into view. After exposing the cervix, one should assess the nature of the cervico-vaginal secretions and note any obvious findings such as ectropion, polyp, nabothian follicles, congenital transformation zone, atrophy, inflammation and infection, leukoplakia (hyperkeratosis), condylomata, ulcer, growth and any obvious lesions in the vaginal fornices. Following this, excess mucus should be removed gently from the cervix with saline-soaked cotton swabs. Swabbing with dry cotton balls is discouraged, as these may induce traumatic bleeding and subepithelial petechiae. Loss of epithelium and bleeding due to rough and traumatic manipulation of the speculum and swabs should be avoided.
Obtain a cervical cytology smear, if necessary
It is likely that the woman has been referred because of an abnormal cytology result; it is, therefore, debatable whether a repeat smear is necessary in such instances. On the other hand, if the colposcopist is interested in the results of a repeat cytology test, the cervix should be sampled for the smear before the application of any solution, such as acetic acid. Sometimes the process of taking a smear will cause bleeding, but this usually subsides gradually after acetic acid is applied.
Obtain specimens for laboratory examination, if necessary
Any necessary swab for screening or diagnostic work-up because of suspicious signs or symptoms should be done at this stage. For example, a swab for Neisseria gonorrhoeae culture can be obtained from the endocervical canal or pus in the vaginal fornix, and a Chlamydia trachomatis specimen can be obtained from the endocervical canal after excessive mucus has been removed. If an ulcerative lesion is found on the vagina or cervix or on the external anogenital area, the colposcopist should consider the possibility of one or more sexually transmitted infections as the cause and the appropriate work up should be performed. If a sample is required to test for example for human papillomavirus (HPV), the cervical cells should be obtained before application of acetic acid.
Following this, the cervix should be inspected at low-power magnification (5x to 10x), looking for any obvious areas of abnormality (e.g., leukoplakia).
Following this, the cervix should be inspected at low-power magnification (5x to 10x), looking for any obvious areas of abnormality (e.g., leukoplakia).
Apply normal saline solution
Normal saline is applied to the cervix with a sprayer or cotton balls and excess liquid is removed afterwards. This is not only the ideal way to conduct a preliminary inspection for surface abnormalities (e.g., leukoplakia, condylomata), but also the best way to examine the detail of cervical capillaries and surface blood vessels. The examination of the blood vessels is further aided by using the green (or blue) filter on the colposcope to enhance the contrast of the vessels, and by using higher levels of magnification (about 15x). Although some experienced colposcopists do not routinely perform an examination after saline has been applied (instead going directly to the application of acetic acid), it has been argued that an examination should be done in all cases, since the information obtained on the location of abnormal vessels can be noted and integrated with the findings from later steps, which will determine the appropriate biopsy site(s), if any. The application of acetic acid, and even Lugols iodine solution, to the cervix can result in tissue swelling and consequent opacity. This swelling and opacity tend to obscure some of the details of the vessels in the subepithelial tissue, so it is always is best to assess the capillaries and vessels with saline before the application of any other solution.
The other important task at this step is to identify the distal and proximal borders of the transformation zone. The inner border is defined by the entire 360-degree circumference of the squamocolumnar junction. If the junction is proximal to the external os, in the canal, it requires additional effort to visualize the entire junction. Opening the blades of the vaginal speculum and using a cotton-tipped applicator to pry the anterior lip up or the posterior lip down will often allow visualization if the junction is close enough to the os. The endocervical speculum (Figure 4.6) or the lips of a long dissection forceps can also be used, and often will allow a greater length of canal to be inspected. The skill for these manoeuvres comes with practice. If the squamocolumnar junction is not visualized in its entire circumference, the colposcopic procedure is termed inadequate or unsatisfactory (see Chapter 6).
The distal limit of the transformation zone, namely the location of the original squamocolumnar junction, may be identified by finding the most distal crypt openings or nabothian follicles in the lips of the cervix and by drawing an imaginary line connecting these landmarks (Figure 5.1).
 figure 4.6: Endocervical speculum<...
figure 4.6: Endocervical speculum<... FIGURE 5.1: A method of identifyin...
FIGURE 5.1: A method of identifyin...Apply acetic acid
This step may be carried out using 3-5% dilute glacial acetic acid. We prefer to use 5% dilute acetic acid as the acetowhite changes may occur faster and be more obvious than with a 3-4% solution. If white table vinegar is used, it is usually 5% acetic acid, but it is preferable to confirm the strength of the solution. The two main purposes of applying acetic acid are, first, to conduct another inspection of the entire new squamocolumnar junction and second, to detect and evaluate any areas of abnormal or atypical transformation zone (ATZ). Acetic acid should be liberally applied to the cervix with a cotton-tipped swab or cotton balls or using a 2 x 2 inches gauze or with a sprayer so that it covers the entire cervical surface, including the external os.
Wiping the cervix a few times with a cotton ball or other large applicator assists in the coagulation and removal of mucus, which in turn helps the acetic acid to penetrate to the epithelium in full strength. The mucus in the canal may be difficult to extract, but it can be easily and temporarily pushed into the os with an acetic acidsoaked cotton swab, particularly if it is obscuring the assessment of an important feature, such as the squamocolumnar junction. In the latter case, the swab also helps to apply the acid to the area of the squamocolumnar junction, which may be just inside the os, and can also be used to manipulate the cervix to view otherwise hidden areas of interest. Patience is required during this step because the acetowhitening effect of acetic acid develops gradually over the course of 60 seconds and the effect may fade afterwards. Hence, acetic acid may be reapplied every 2 to 3 minutes during the examination. A swab may be used to reapply, using the acetic acid pooled in the posterior aspect of the vagina.
Wiping the cervix a few times with a cotton ball or other large applicator assists in the coagulation and removal of mucus, which in turn helps the acetic acid to penetrate to the epithelium in full strength. The mucus in the canal may be difficult to extract, but it can be easily and temporarily pushed into the os with an acetic acidsoaked cotton swab, particularly if it is obscuring the assessment of an important feature, such as the squamocolumnar junction. In the latter case, the swab also helps to apply the acid to the area of the squamocolumnar junction, which may be just inside the os, and can also be used to manipulate the cervix to view otherwise hidden areas of interest. Patience is required during this step because the acetowhitening effect of acetic acid develops gradually over the course of 60 seconds and the effect may fade afterwards. Hence, acetic acid may be reapplied every 2 to 3 minutes during the examination. A swab may be used to reapply, using the acetic acid pooled in the posterior aspect of the vagina.
Apply Lugols iodine solution
Normal squamous (both original and mature metaplastic) epithelial cells contain stores of glycogen that give a mahogany brown or nearly black stain when an iodine-containing solution, such as Lugols, is applied. In contrast, normal columnar epithelium does not contain glycogen and does not take up the iodine stain. Similarly, immature squamous metaplasia, inflammatory and regenerating epithelium and congenital transformation zone contain very little or no glycogen and either do not or only partially stain with iodine. Condylomata also either do not or only partially stain with iodine. Abnormal transformation zones, such as those with CIN or invasive cancer, contain very little or no glycogen. The degree of differentiation of the cells in a preneoplastic squamous lesion determines the amount of intracellular glycogen and thus the degree of staining observed. Therefore, one would expect to see a range of staining from partially brown to mustard yellow across the spectrum from low- to high-grade CIN. Usually high-grade CIN takes up less of the stain, appearing as mustard or saffron yellow areas. In the case of high-grade CIN, vigorous or repeated application of iodine may occasionally peel off the abnormal epithelium and the underlying tissue stroma may appear pale, as it lacks glycogen.
It is important always to integrate the findings of the saline, acetic acid, and iodine tests to make a colposcopic assessment. The iodine test is also very helpful for determining whether vaginal lesions are present. Application of iodine will clearly delineate the borders of a lesion before a biopsy, or treatment of the lesion, is attempted.
It is important always to integrate the findings of the saline, acetic acid, and iodine tests to make a colposcopic assessment. The iodine test is also very helpful for determining whether vaginal lesions are present. Application of iodine will clearly delineate the borders of a lesion before a biopsy, or treatment of the lesion, is attempted.
Perform cervical biopsies, if necessary
Once an abnormal transformation zone is detected, the area is evaluated and compared with other areas of the cervix. If any other abnormal zones are present, the colposcopist should then decide from where a biopsy or biopsies should be taken. It is essential to obtain one or more directed punch biopsies from areas colposcopically identified as abnormal and/or doubtful. Biopsy should be obtained from the area of the lesion with worst features and closest to the squamocolumnar junction. Biopsy always should be done under colposcopic control by firmly applying the biopsy instrument (Figure 4.8), with the jaws wide open (Figure 5.2), to the cervical surface to be sampled. The cervix may move back somewhat with this manoeuvre, but that is normal.
To obtain a tissue sample, the biopsy forceps is guided under colposcopic visualization to the area from which the tissue specimen is to be obtained. The cervix may tend to slip away on pressure, but it is usually easy to grasp and remove tissue if the forceps used for biopsy has wide and sharp cutting edges, with one or two teeth to anchor the forceps while taking the biopsy (Figure 5.2). A tenaculum may be also used to fix the cervix before taking the biopsy. The jaws are then closed completely, and the specimen is removed and immediately placed in formalin. The biopsy performed should be deep enough to obtain adequate stroma, in order to exclude invasion. Cutting the specimen should be carried out by quick and firm closure of the jaws. Repeated cutting and rotation of the forceps should be avoided, as they can crush the tissue sample. The procedure is usually painless if carried out efficiently using a sharp and toothed biopsy forceps. A skin hook is sometimes useful to anchor a potential biopsy site if it is difficult to grasp with the biopsy instrument. After the biopsy has been obtained, it is advisable to indicate the site of the target area which has been biopsied, on the diagram of cervix in the reporting form. It is important to place the freshly obtained biopsy specimen in a labelled bottle containing 10% formalin. The biopsy site(s) may be cauterized with Monsels paste or with a silver nitrate stick immediately after the procedure to control any bleeding.
To obtain a tissue sample, the biopsy forceps is guided under colposcopic visualization to the area from which the tissue specimen is to be obtained. The cervix may tend to slip away on pressure, but it is usually easy to grasp and remove tissue if the forceps used for biopsy has wide and sharp cutting edges, with one or two teeth to anchor the forceps while taking the biopsy (Figure 5.2). A tenaculum may be also used to fix the cervix before taking the biopsy. The jaws are then closed completely, and the specimen is removed and immediately placed in formalin. The biopsy performed should be deep enough to obtain adequate stroma, in order to exclude invasion. Cutting the specimen should be carried out by quick and firm closure of the jaws. Repeated cutting and rotation of the forceps should be avoided, as they can crush the tissue sample. The procedure is usually painless if carried out efficiently using a sharp and toothed biopsy forceps. A skin hook is sometimes useful to anchor a potential biopsy site if it is difficult to grasp with the biopsy instrument. After the biopsy has been obtained, it is advisable to indicate the site of the target area which has been biopsied, on the diagram of cervix in the reporting form. It is important to place the freshly obtained biopsy specimen in a labelled bottle containing 10% formalin. The biopsy site(s) may be cauterized with Monsels paste or with a silver nitrate stick immediately after the procedure to control any bleeding.
 figure 4.8: Cervical punch biopsy ...
figure 4.8: Cervical punch biopsy ... figure 5.2: Biopsy technique: A to...
figure 5.2: Biopsy technique: A to...Apply Monsels paste after biopsy
It is usual practice to ensure haemostasis by applying Monsels (ferric subsulfate) paste to the biopsy site. This is done by gently applying pressure with a cotton-tipped applicator, the tip of which has been coated with Monsels paste (see Appendix 3). Monsels solution is the most common haemostatic agent used after cervical biopsy or excision, and it performs well when it has a thick, toothpaste-like consistency. The paste-like consistency may be produced by exposing the stock solution to the air in a small container, which results in evaporation and thickening of the agent, or using a microwave oven. The paste-like consistency may be preserved by keeping the paste in a closed container and by adding small amount of Monsels solution whenever it becomes dry and excessively thick.
A silver nitrate stick can also be used to cauterize a biopsy site. The haemostatic action of these chemicals is much better if the chemical is applied promptly, before bleeding begins, allowing direct contact of the chemical with the tissue rather than with blood.
A silver nitrate stick can also be used to cauterize a biopsy site. The haemostatic action of these chemicals is much better if the chemical is applied promptly, before bleeding begins, allowing direct contact of the chemical with the tissue rather than with blood.
Perform endocervical curettage, if necessary
There are three commonly encountered circumstances, in which an endocervical curettage (ECC) should be performed using an endocervical curette (Figure 4.7). First, if the colposcopic examination of the ectocervix has not revealed any abnormality, yet the woman has been referred because of a cytological abnormality, an ECC should be performed to properly evaluate the endocervical canal, which may contain a hidden invasive cancer or other lesion. Second, if the referral cytology indicated that a glandular lesion may be present, an ECC should be performed (regardless of the findings of the colposcopic examination). Third, an ECC should be performed if the colposcopic examination has been unsatisfactory (whether or not a cervical lesion has been detected). However, it should be mentioned that the yield of an ECC is very low in inexperienced hands, as it is frequently associated with inadequate tissue sampling. Thus, in such situations, a negative ECC should not be taken as unequivocal evidence of the absence of neoplasia in the endocervical canal.
In the above three situations, and particularly in the case of an acetowhite lesion extending into the canal, it may be prudent to excise the cervix with a cone (by LEEP or cold knife conization, as appropriate; see Chapter 11 and Chapter 13). However, this approach places a large work load on histopathology services and, as such, may not be feasible in several sub-Saharan African countries and other developing regions with extremely limited or even no histopathology services. In the assessment of women in such settings, it is left to the discretion of the colposcopist to decide whether an ECC and/or cone biopsy should be performed. Due to the risk of an adverse effect on pregnancy outcome, ECC is absolutely contraindicated in pregnant women.
Before ECC is performed, the posterior fornix must be dry to avoid the loss of curetted tissue in the acetic acid solution which accumulated during its application on the cervix. When performing ECC, the colposcopist holds the curette like a pen and scrapes the endocervical canal in firm, short, linear strokes until it has been completely sampled. During the procedure the curette should remain in the canal. When extracting the curette, care should be taken to twirl it in order to encourage the contents of the curette basket to remain trapped therein. The curettings should be put onto a piece of either gauze or brown paper, and then promptly placed into formalin. Any residual tissue can be removed from the canal with forceps. In order to avoid the potential confusion of inadvertently sampling a visible lesion on the ectocervix or including residual tissue from an ectocervical biopsy in the neighbourhood of the external os in the endocervical curette specimen, some colposcopists perform ECC under colposcopic control, before obtaining a cervical biopsy.
In the above three situations, and particularly in the case of an acetowhite lesion extending into the canal, it may be prudent to excise the cervix with a cone (by LEEP or cold knife conization, as appropriate; see Chapter 11 and Chapter 13). However, this approach places a large work load on histopathology services and, as such, may not be feasible in several sub-Saharan African countries and other developing regions with extremely limited or even no histopathology services. In the assessment of women in such settings, it is left to the discretion of the colposcopist to decide whether an ECC and/or cone biopsy should be performed. Due to the risk of an adverse effect on pregnancy outcome, ECC is absolutely contraindicated in pregnant women.
Before ECC is performed, the posterior fornix must be dry to avoid the loss of curetted tissue in the acetic acid solution which accumulated during its application on the cervix. When performing ECC, the colposcopist holds the curette like a pen and scrapes the endocervical canal in firm, short, linear strokes until it has been completely sampled. During the procedure the curette should remain in the canal. When extracting the curette, care should be taken to twirl it in order to encourage the contents of the curette basket to remain trapped therein. The curettings should be put onto a piece of either gauze or brown paper, and then promptly placed into formalin. Any residual tissue can be removed from the canal with forceps. In order to avoid the potential confusion of inadvertently sampling a visible lesion on the ectocervix or including residual tissue from an ectocervical biopsy in the neighbourhood of the external os in the endocervical curette specimen, some colposcopists perform ECC under colposcopic control, before obtaining a cervical biopsy.
 figure 4.7: Endocervical curette
figure 4.7: Endocervical curetteInspect vaginal walls, vulva, perineum, and perianal areas
As the speculum is withdrawn, the vaginal walls and, subsequently, the vulvar, perineal, and perianal epithelium should be inspected. The surfaces are bathed with acetic acid and after one or two minutes the acetowhite areas are noted and evaluated. There is no general agreement on whether these areas should be routinely examined in this fashion, but it seems sensible, given that the examination adds very little time and effort, and that HPV has a propensity to infect these areas and cause intraepithelial lesions, most of which are treatable.
Bimanual and rectal examination
Some practitioners believe that bimanual and rectal examination should be performed before colposcopy, some believe that it should be done after, and some do not include it as a part of the normal colposcopy clinic protocol. If it is performed before colposcopy, only water should be used as a lubricant. Despite this lack of agreement, bimanual and rectal examination can provide information about the orientation of the axis of the vaginal canal before insertion of the vaginal speculum, and it allows palpation of the cervix to detect signs of nodularity or hardness and masses in other pelvic structures, such as the ovaries and uterus. It has been argued that knowledge of other abnormalities, such as sizeable uterine fibroids, can play a role in planning the best therapy for a woman.
Explain the findings to the woman
After the woman has dressed, carefully explain the examination findings and offer her the opportunity to ask questions. Review the management plan, emphasize the importance of adequate follow-up, and discuss any barriers to compliance.
Document the findings
The findings of the colposcopic examination should be recorded with the aid of appropriate forms that are filed in such a way as to be easily retrievable.
If the woman is pregnant
The effects of pregnancy on the cervix are oedema, an increase in the area of the epithelium, enlargement and opening of the os, and eversion. As pregnancy progresses, these changes are exaggerated, so that an inadequate examination at the beginning of pregnancy may become adequate by a later stage due to eversion. Certain difficulties in examination, however, become more pronounced as pregnancy progresses: the vaginal walls tend to be redundant and collapse, obscuring the view; cervical mucus is increased; increased vascularity leads to easily induced bleeding; the blood vessel pattern in cervical pseudo-decidual tissue tends to mimic invasive cancer; and CIN tends to appear as a more severe grade than it actually is (due to increased size, increased oedema and vasculature pattern). Thus considerable experience is required for colposcopy in pregnancy.
The steps in the colposcopic procedure for a pregnant woman are similar to those for a non-pregnant woman, but extra care must be taken not to injure any tissues when a digital examination or speculum insertion is performed. If a repeat cytology smear is needed, this may be performed using a spatula, by applying gentle pressure to avoid bleeding. Some may prefer to obtain a cytology sample at the end of the colposcopic procedure, in order to avoid inducing bleeding that may obscure the colposcopic field, but this may result in a poor hypocellular sample, as cells might have been washed away during the different steps of the colposcopic procedure.
As pregnancy progresses, cervical biopsy is associated with an increased probability and degree of bleeding, which may often be difficult to control. The risk of biopsy should always be weighed against the risk of missing an early invasive cancer. All lesions suspicious of invasive cancer must be biopsied or wedge excised. Sharp biopsy forceps should be used, as they will produce less tearing of tissue. Biopsy should always be carried out under colposcopic vision to control depth. The prompt application of Monsels paste or silver nitrate to the biopsy site, immediate bed rest for 15 to 30 minutes, and the use of a tampon or other haemostatic packing to put pressure on the biopsy site are helpful to minimize bleeding. Some women may need an injection of pitressin into the cervix or suturing for haemostasis. To avoid a large amount of tissue slough, due to the effect of Monsels paste, haemostatic packs should not be left in place for more than a few hours after the paste has been applied. Alternatively, cervical biopsy in a pregnant woman may be performed with diathermy loop. If colposcopy is inadequate, and cytology suggests invasive cancer, a conization must be performed, ideally in the second trimester. Non-invasive lesions may be evaluated post-partum.
The steps in the colposcopic procedure for a pregnant woman are similar to those for a non-pregnant woman, but extra care must be taken not to injure any tissues when a digital examination or speculum insertion is performed. If a repeat cytology smear is needed, this may be performed using a spatula, by applying gentle pressure to avoid bleeding. Some may prefer to obtain a cytology sample at the end of the colposcopic procedure, in order to avoid inducing bleeding that may obscure the colposcopic field, but this may result in a poor hypocellular sample, as cells might have been washed away during the different steps of the colposcopic procedure.
As pregnancy progresses, cervical biopsy is associated with an increased probability and degree of bleeding, which may often be difficult to control. The risk of biopsy should always be weighed against the risk of missing an early invasive cancer. All lesions suspicious of invasive cancer must be biopsied or wedge excised. Sharp biopsy forceps should be used, as they will produce less tearing of tissue. Biopsy should always be carried out under colposcopic vision to control depth. The prompt application of Monsels paste or silver nitrate to the biopsy site, immediate bed rest for 15 to 30 minutes, and the use of a tampon or other haemostatic packing to put pressure on the biopsy site are helpful to minimize bleeding. Some women may need an injection of pitressin into the cervix or suturing for haemostasis. To avoid a large amount of tissue slough, due to the effect of Monsels paste, haemostatic packs should not be left in place for more than a few hours after the paste has been applied. Alternatively, cervical biopsy in a pregnant woman may be performed with diathermy loop. If colposcopy is inadequate, and cytology suggests invasive cancer, a conization must be performed, ideally in the second trimester. Non-invasive lesions may be evaluated post-partum.



