Image | Caption |
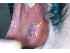 | Figure 1: Annular form of lichen planus on the right buccal mucosa. Note the pigmentation and the ring-like pattern of Wickham striae (yellow arrows). |
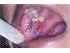 | Figure 2: Annular form of lichen planus on the right buccal mucosa. Note the ring-like pattern of Wickham striae (red arrows). |
 | Figure 3: Annular form of lichen planus on the right buccal mucosa. Note the ring-like pattern of white striae (yellow arrows). |
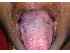 | Figure 4: Lichen planus. Note the white 4x3.5 cm patch on the right side of the dorsum tongue intermingled with areas of pigmentation. Another annular form of lichen planus can be seen on the left side of the dorsum tongue. |
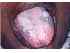 | Figure 5: Lichen planus. Note the diffuse areas of pigmentation of the dorsum tongue intermingled with Wickham striae. The individual papillae on the tongue can be made out distinctly. |
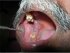 | Figure 6: Annular lichen planus. Note the ring-like pattern on the right buccal mucosa, retromolar trigone and hard palate. |
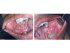 | Figures 7: A reticular form of lichen planus. Note the bilaterally symmetrical patterns, which are characteristic of lichen planus. |
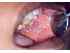 | Figure 8: Lichen planus. Note the reticular arrangement of Wickham striae on the left buccal mucosa of this 30year-old female patient. |
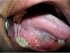 | Figure 9: Reticular lichen planus involving the posterior ventrolateral aspect of the tongue. Note the prominent lingual varicosities anteriorly. |
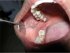 | Figure 10: Reticular lichen planus involving right buccal mucosa and dorsum of the tongue. |
 | Figure 11: Reticular lichen planus. Note the extensive lesions involving right buccal mucosa and retromolar trigone. |
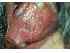 | Figure 12: Lichen planus in the right buccal mucosa. Note the lacy white Wickham striae and the localized hyperpigmentation. |
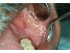 | Figure 13: Lichen planus in the left buccal mucosa. Note the Wickham striae posteriorly (yellow arrow) and the Fordyce granules anteriorly (red arrows), which appear as small yellow nodules. |
 | Figure 14: Lichen planus. Fig. 14A: Note the small papules on the dorsum tongue (yellow arrow) intermingled with areas of pigmentation. Fig. 14B: Cutaneous involvement of lichen planus. Note the well-defined macular lesions on the legs of the same person with oral manifestations of lichen planus. |
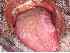 | Figure 15: Lichen planus of the tongue. |
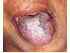 | Figure 16: Plaque type lichen planus. Note the 4x3 cm raised lesion on the dorsum of the tongue surrounded by hyperpigmentation. |
 | Figure 17: Bullous or vesicular lichen planus. Note the fluid-filled vesicles, which project out from the surface (arrow). |
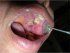 | Figure 18: Atrophic lichen planus. Note the extensive nature of the atrophic lichen planus involving the hard palate, retromolar trigone, buccal mucosa, labial mucosa and tongue. |
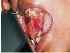 | Figure 19: Erosive Lichen Planus. An erosive lesion of 2x1 cm size on the right buccal mucosa surrounded by Wickham striae. |
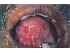 | Figure 20: Erosive lichen planus on the ventral surface of the tongue, just above the lingual frenum, surrounded by white striae. |
 | Figure 21: Erosive lichen planus. An erosive area of 1x1 cm on the right buccal mucosa, surrounded by Wickham striae. |
 | Figure 22: Erosive lichen planus. Note the erosive patch on the left buccal mucosa surrounded by Wickham striae. |
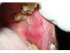 | Figure 23: Erosive lichen planus. Note the areas of erosion interspersed with Wickham striae on the left buccal mucosa. |
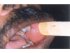 | Figure 24: Lichenoid reaction (arrow) in this pan masala chewer. Note the white striae on the left buccal mucosa. |
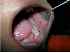 | Figure 25: Lichenoid reaction. Note the lichenoid reaction on the left buccal mucosa due to type IV hypersensitivity reaction to amalgam filling in the buccal aspect of first and second molars on the left lower jaw. |